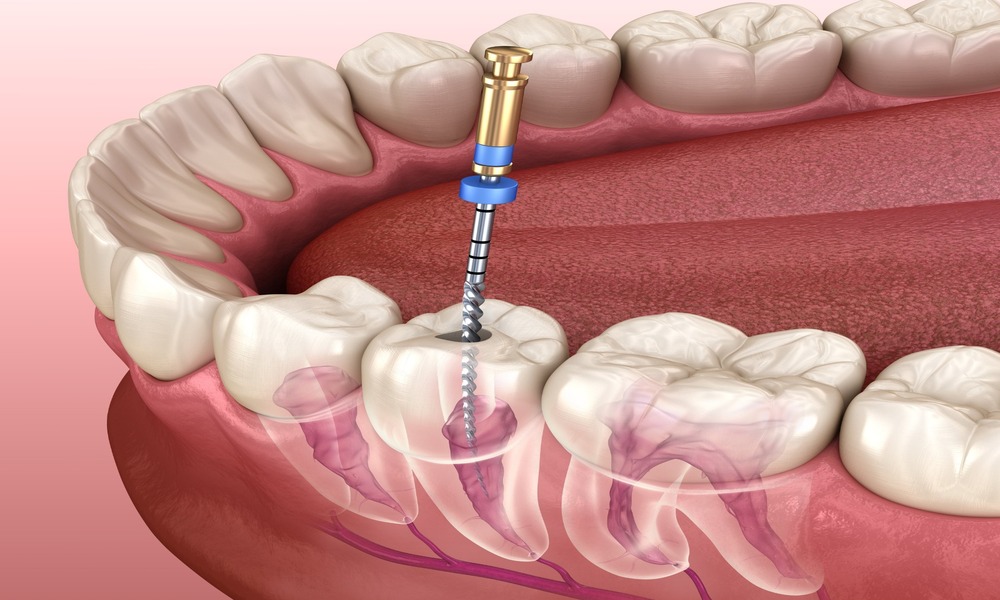
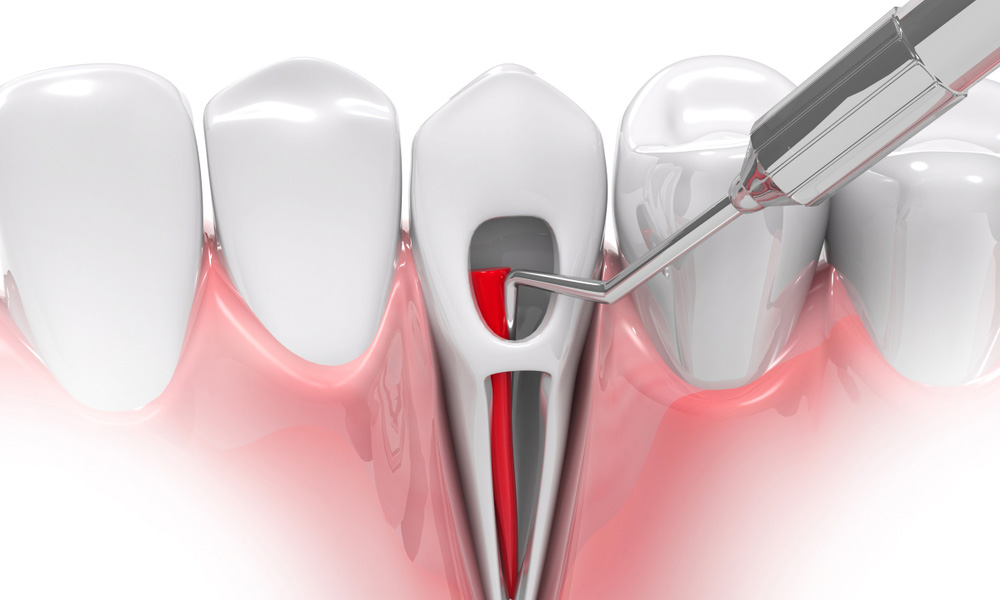
A root canal treatment is designed to save a severely infected or damaged tooth by removing infected pulp and sealing the inner structure. In most cases, it is highly successful and lasts for years or even a lifetime. However, there are situations where the initial treatment does not fully resolve the problem, leading to the need for a second procedure, commonly known as root canal retreatment.
Understanding the warning signs early can help prevent complications and save your natural tooth before the condition worsens.
Why a Second Root Canal May Be Needed
A second root canal is required when the treated tooth becomes reinfected or fails to heal properly. This can happen due to several reasons such as missed canals during the initial procedure, incomplete cleaning, delayed crown placement, or new decay that exposes the treated area.
In some cases, complex tooth anatomy or cracks can also allow bacteria to re-enter the tooth, leading to recurring infection.
Common Signs That Indicate the Need for Retreatment
Recognizing the symptoms early is crucial. Here are the most common signs that may suggest you need a second root canal procedure.
Persistent or Recurring Pain
Pain that continues long after your initial root canal is not normal. While mild discomfort is expected for a few days, ongoing or returning pain weeks or months later may indicate that the infection was not completely removed.
The pain may be dull, sharp, or triggered by biting or chewing.
Sensitivity to Hot and Cold
A tooth that has undergone a root canal should not respond to temperature changes. If you start feeling sensitivity to hot or cold again, it may be a sign that some nerve tissue or infection remains inside the tooth.
This sensitivity can range from mild discomfort to sharp pain.
Swelling in the Gums or Face
Swelling around the treated tooth is a clear sign of inflammation or infection. It may appear as puffiness in the gums, cheek, or jaw area.
In some cases, the swelling may come and go, which often indicates a chronic infection that flares up periodically.
Gum Boil or Pimple Near the Tooth
A small bump or pimple on the gums, often referred to as an abscess, is one of the most noticeable signs of infection. It may release pus and can be associated with a bad taste or odor in the mouth.
Even if the pimple disappears temporarily, the infection may still be present beneath the surface.
Tooth Discoloration
Darkening of a previously treated tooth can indicate internal damage or infection. While some discoloration is normal after a root canal, a sudden or worsening change in color should not be ignored.
This may signal that the tooth is not healing as expected.
Pain When Biting or Chewing
If you feel discomfort or pressure when biting down, it could mean that the infection has spread to the surrounding bone or tissues.
This type of pain is often localized and becomes more noticeable during meals.
Delayed Healing or No Improvement
After a root canal, symptoms should gradually improve within a few days to weeks. If your tooth does not feel better or symptoms persist, it may indicate treatment failure.
A lack of healing is often detected during follow-up dental visits or X-rays.
Cracked or Damaged Tooth
A crack in the treated tooth can allow bacteria to enter again, leading to reinfection. Even a small fracture can compromise the seal created during the initial procedure.
If the tooth feels sensitive or unstable, it should be examined immediately.
Loose Crown or Filling
A crown or filling placed after a root canal protects the tooth from bacteria. If it becomes loose, damaged, or falls off, the inner structure is exposed to infection.
This significantly increases the risk of needing retreatment.
Causes Behind Root Canal Failure
Several factors can contribute to the failure of a root canal treatment.
Complex root canal anatomy where tiny canals were missed
Incomplete cleaning or sealing of the canals
Delay in placing a permanent restoration
New cavities forming around the treated tooth
Cracks or fractures in the tooth structure
Poor oral hygiene or neglect
Understanding these causes helps in preventing future issues after retreatment.
What Happens During a Second Root Canal
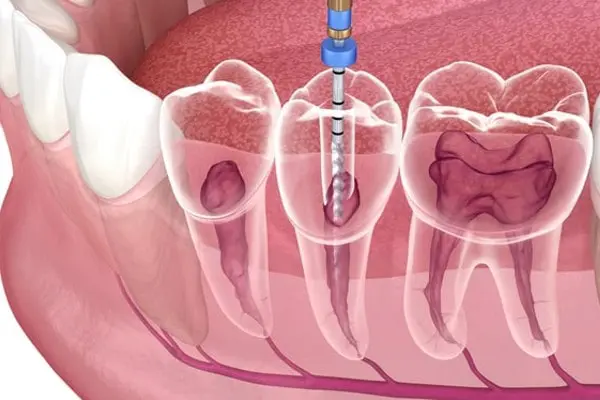
A second root canal procedure involves reopening the tooth, removing the previous filling material, and thoroughly cleaning the canals again. The dentist will locate any missed or infected areas, disinfect the canals, and reseal them properly.
In some cases, advanced imaging or magnification tools are used to ensure complete cleaning. After the procedure, a new crown is usually placed to protect the tooth.
Is Retreatment Successful
Root canal retreatment has a high success rate when performed correctly. Many teeth can be saved and continue to function normally for years.
However, success depends on the condition of the tooth, the extent of infection, and how early the problem is addressed.
When Extraction May Be Considered
If the tooth is severely damaged, cracked beyond repair, or the infection is too advanced, extraction may be recommended as a last resort. The missing tooth can then be replaced with options such as implants or bridges.
The goal is always to preserve the natural tooth whenever possible.
How to Prevent the Need for a Second Root Canal
Prevention plays a key role in avoiding retreatment.
Maintain proper oral hygiene by brushing and flossing daily
Visit your dentist regularly for checkups and cleanings
Get a crown placed promptly after a root canal
Avoid chewing hard foods that may crack the tooth
Address cavities or dental issues early
Follow post-treatment care instructions carefully
Taking these steps significantly reduces the risk of reinfection.
Final Thoughts
A root canal is a reliable treatment, but it is not immune to failure. Recognizing the signs of a problem early can help you seek timely care and avoid complications. Persistent pain, swelling, sensitivity, or changes in the treated tooth should never be ignored.
If you suspect something is wrong, consult your dentist immediately. With proper diagnosis and retreatment, most teeth can be saved and restored to full function, ensuring long-term oral health.